PADI IDC Revision Dive Theory
Physiology
Buy the IDC revision packs that now include ten practice exams, the exams include all the questions and answers you will need to revise to PASS the PADI IDC and IE, we even have more Physiology Revision for you.
Ears & Sinuses
The ear is not only an organ of hearing but also one of regulating equilibrium
Inner Ear:
Very delicate and protected
Cochlea – Liquid filled
Oval Window – Ossicles are attached to the oval window (flexes to vibration) of the cochlea
Round Window – Compensates pressure, flexing opposite to the oval window
Vestibular canals – Control balance and orientation
Middle Ear:
Most affected by changing pressure, such as when you are in an aircraft and swallowing relieves the pressure.
When diving, if equalization doesn’t occur then the ear drum (tympanic membrane) could tear or rupture leading to fluid in the middle ear, therefore never force equalizations and equalize often and early.
Responses to dive pressures – only one with air pocket
Sound waves vibrate the eardrum (attached to the ossicles)
Vibrations go from eardrum to ossicles to cochlea (inner ear)
Outer Ear:
The visible fleshy part of the ear
Always equalized as open to environment
Traps sound waves and channels them to middle ear, via ear canal to the ear drum
Take another look at the ear diagrams. Try to remember the names of the parts. Remember that the middle ear is the part most affected by pressure. Imagine describing the ear and pressure to a student, once you can do this you will be better able to answer questions on this subject.
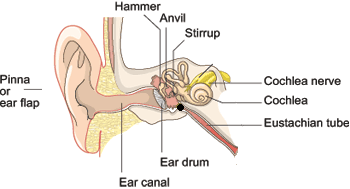
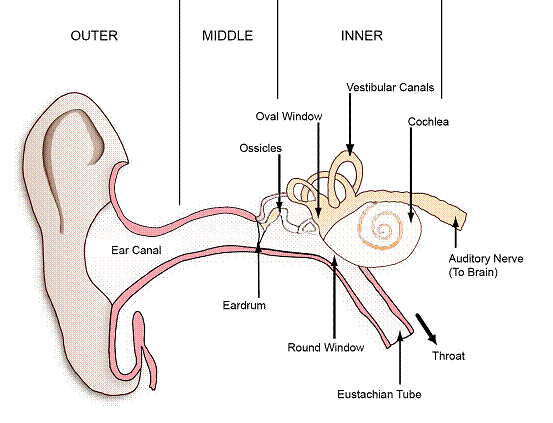
The auditory nerve is known as the vestibular-cochlear nerve, it goes straight to brainstem.
CHANGING PRESSURE When descending, increasing pressure pushes in on the eardrum – if equalisation doesn’t take place then the diver feels discomfort. By equalising, the diver forces air up the Eustachian tube to equalize the pressure, alleviating the discomfort. Expanding air normally exits the Eustachian tube easily – seldom required to do anything during ascent.
Problems in body air spaces.
BAROTRAUMA
Barotrauma means ‘pressure injury’, and results when a body air space isn’t equalized and pressure continues or increases.
MIDDLE EAR SQUEEZE
Causes:
Failure to equalize or inability to equalize due to congestion, diving with a cold)
Signs and Symptoms:
Sharp pain caused by the hydrostatic pressure forcing the eardrum inward towards the airspace with less pressure (i.e. inside your ear)
EARDRUM RUPTURE
Causes:
Failure to equalize, but pressure increases faster than fluids can fill the middle ear. The eardrum tears due to pressure.
Signs and Symptoms:
Usually heals without complication, but requires medical attention to prevent infection and permanent damage because water contaminates the ear with organic matter and dirt.
REVERSE SQUEEZE
Ears equalize on decent but congestion at depth prevents air from escaping during ascent. Eardrum flexes outward
Causes:
Usually caused by diving with a cold using decongestants (decongestant wears off during dive causing blockage)
Signs and symptoms:
- Reduced hearing
- Vertigo
- Balance problems
- Ear ringing
- A feeling that the ears are blocked
This is a serious injury requiring medical treatment to avoid or reduce permanent hearing damage.
ROUND WINDOW RUPTURE
Causes:
Caused by delayed equalization accompanied by forceful Valsalva manoeuvre (exhaling against pinched nostrils).
Signs and symptoms:
Valsalva raises pressure in thorax, which causes increase in pressure in cochlea (connected by fluid as part of the nervous system). This plus transmitted pressure bursts round window outward.
VERTIGO
Occurs when the eardrum ruptures and cold water on the vestibular canals cause momentary loss of sense of direction and dizziness
Circulatory System
The circulatory system transports oxygen fuel and materials from the respiratory and digestive systems to your body tissues. It carries waste carbon dioxide and other material wastes from your tissues for elimination. The transport of gases to and from the respiratory system is the most urgent function, and the one most relevant to diving. The components of the respiratory (circulatory) system include:
Heart
Four-chambered organ made of specialised muscle pumps that pump oxygenated blood through arteries to tissues throughout the body.
Arteries / Capillaries
Arteries are elastic vessels that carry blood away from the heart, branch into capillaries, the body’s smallest blood vessels, where the bloodstream and tissues exchange gas and nutrients.
Veins
Receive deoxygenated blood from the capillaries, returning it back to the respiratory system and heart to exchange gases in the lungs and repeat the cycle.
Heart Rate
The pulse rate measures the frequency of the heart rate. An average adults at rest has a heart rate of 60 to 80 beats per minute. Medically, tachycardia is more than 100bpm, bradycardia less than 60 bpm.
Blood pressure
Blood flows into the arterial system in pressure surges that coincide with heart contractions. The systolic pressure is the surge or high point as the heart contracts. Diastolic pressure is the lull after the surge, or low point when the heart relaxes and fills with blood from the lungs, ready to be pumped around the body with the next contraction.
Adrenaline
During stress or fright, the adrenal gland (which sit on top of the kidneys) releases adrenaline into the circulatory system as part of the survival response of the body. Adrenaline stimulates the heart, constricts blood vessels, and increases the breathing rate to prepare the body to flee or fight a threat.
Blood
Blood consists of several components to accomplish its different functions:
Plasma
Liquid that carries nutrients, chemicals and dissolved gases i.e. carbon dioxide waste & nitrogen.
Red Blood Cells
Carry the majority of oxygen required via haemoglobin (a protein that bonds with oxygen) only 0.001% of O2 dissolved)
Haemoglobin
Blood circulates through lungs, where higher oxygen pressure enables better bonding with haemoglobin, which is then released to the tissues. Once released it picks up carbon dioxide (in the plasma in the form of bicarbonate) and transports it to the lungs for elimination. Carries and releases oxygen efficiently because variations in oxygen partial pressure influences its capacity to remain bonded with oxygen. If the haemoglobin is damaged then the blood would need to circulate 20 times faster to supply the tissues with oxygen.
5% of carbon dioxide the blood carries is in solution in the plasma, 20% combines with haemoglobin and 75% transports in the form of bi-carbonates.
8% CO2 carried in solution arterial system, 10% carried in solution to lungs in venous system,5% as carbaminohaemoglobin arterial blood, 30% in venous system, 87% CO2 carried as bicarb arterial blood, 60% venous blood- not sure how much detail you want,but the venous carriage probably more important to include as there is more CO2 and it’s the venous system which gets rid of CO2.
RESPIRATORY SYSTEM
Your respiratory system integrates with your cardiovascular system by providing your blood with the environment it needs for gas exchange. The respiratory system consists of passages and organs that bring atmospheric air into the body. The components of the respiratory system include the oral-nasal passage, pharynx, larynx, trachea, bronchi, bronchioles, alveolar ducts, and alveoli
Oral / nasal passage
The oral-nasal passage includes the mouth and nasal cavities. The nasal passages are lined with a mucous membrane that contains many fine, ciliated hair cells. The membrane’s primary purpose is to filter air as it enters the nasal cavity. The hairs continually clean the membrane by sweeping filtered material to the back of the throat where it is either swallowed or expelled through the mouth. Therefore, air that enters through the nasal cavity is better filtered than air that enters through the mouth.
Pharynx
The pharynx, the back of the throat, is connected to the nasal and oral cavities. It primarily humidifies and warms the air entering the respiratory system.
Trachea
The trachea, or windpipe, is a tube through which air moves down into the bronchi. From there, air continues to move down increasingly smaller passages, or ducts (bronchioles), until it reaches the small alveoli within the lung tissue.
Alveoli
The actual gaseous exchange between carbon dioxide and oxygen occurs in the alveoli. The alveoli are surrounded by a network of capillaries that joins veins and arteries. Carbon dioxide and oxygen move in and out of alveoli because of the pressure differentials between their CO2 and O2 levels and those in surrounding capillaries. This movement is based on the law of gaseous diffusion: a gas always moves from an area of high pressure to an area of lower pressure.
Breath Hold Diving
During breath hold diving the circulatory system uses oxygen stored in the lungs, muscles and blood to supply tissues.
Accumulating carbon dioxide creates urges to breathe (via a centre in the brain) and eventually it is too great to ignore, forcing the diver to surface and breathe.
Hyperventilating (3 to 4 times) can increase breath hold time. Doing so reduces circulatory carbon dioxide so it takes longer to accumulate enough to stimulate breathing. Excessive hyperventilation may lead to shallow water blackout.
Shallow Water Blackout
Caused by excessive hyperventilation, depleting a divers carbon dioxide level. At depth, a divers body consumes oxygen faster than carbon dioxide accumulates to stimulate breathing.
Depleted oxygen causes no problem at depth because high pp allows haemoglobin to bond with the remaining supply.
The diver ascends, the pp drops and haemoglobin can no longer bond with oxygen; the diver blacks out without warning due to hypoxia (insufficient oxygen).
Carotid-Sinus Reflex
Arterial blood reaches the brain through the carotid arteries, which branch up each side of the neck. Carotid-sinus receptors monitor blood pressure within the carotid arteries and send impulses to the cardioinhibitory centre in the brain to regulate the heart.
When the carotid-sinus receptors detect high blood pressure, it stimulates the cardioinhibitory centre, which slows the heart rate. When the carotid sinus receptors detect low blood pressure, it stops stimulating the cardioinhibitory centre, which in turn stops sending signals to the heart. The heart rate then increases. Wearing anything tight around the neck could constrict the carotid sinus. This could lead to unconsciousness preceded by light headiness and discomfort.
Nitrogen
When we breathe, from the lungs, our body takes the oxygen and delivers it to the body’s muscles. The body uses oxygen but the body DOES NOT use the nitrogen for anything. This is what we call an inert gas. Nitrogen is an inert gas.
Gas Exchange
Gas exchange between the respiratory and circulatory syste m occurs between the bronchi (alveoli) and the pulmonary capillaries. It is here that the blood releases carbon dioxide and picks up oxygen.
DECOMPRESSION SICKNESS (DCS)
Causes of DCS
Relating to Henry’s Law, if the pressure increases (gets more) the more gas will be dissolved (go into) the liquid. If the pressure is decreased (gets less) the gas will come out of the liquid (the human body is mostly made of liquids). Because the body does not use nitrogen, however when under pressure (diving) our body is exposed to a higher absorption rate of nitrogen (he body has to store this nitrogen within the body) On ascent when diving the pressure on the body is reduced (gets less) and the nitrogen in the body has a higher pressure and has to come out (supersaturation – like when opening a Coca-Cola bottle after shaking it) As long as the nitrogen comes out slowly and is controlled, there is no problem. However, if the pressure is released too fast the nitrogen will come out too fast. This will cause BUBBLES, which cause decompression sickness.
OTHER FACTORS THAT MAY PREDISPOSE A DIVER TO DEVELOP DCS
Fat: Fat releases nitrogen slowly. More nitrogen in solution after a dive.
Age: As we age our circulatory system becomes less efficient.
Dehydration: reduces blood in circulation, slowing nitrogen elimination.
Injuries / illness: may alter or restrict circulation.
Alcohol: before or after diving will alter circulation and causes dehydration.
Carbon Dioxide Excess: from skip breathing.
Cold Water: circulation to the extremities reduces as a diver cools, slowing nitrogen elimination from those areas.
Heavy Exercise: before, during or after a dive accelerates circulation.
Altitude / Flying: dive tables / computers are based on surfacing at sea level, thus exposure to lower pressure increases the tissue pressure gradient.
Types of DCS
TYPE I – identified as ‘pain only’ DCS
Limb pain is the most common – may be mid-limb or joints
Cutaneous DCS (skin bends) – red rashes / patches usually on shoulders and upper chest
TYPE II – identified as having life threatening or immediate injuries
Symptoms – involves brain nervous system, lungs numbness and / or tingling
Paralysis
Weakness / fatigue / nausea (getting sick)
Unconsciousness and death
FIRST AID
Treat all DCS as serious – even pain only
Give patient oxygen – preferably 100% which lowers alveolar nitrogen to accelerate elimination from tissues and raises blood Oxygen levels to assist tissues with blood flow reduced by bubble blockage.
Keep a breathing patient lying down on their left side, with head supported (recovery position) which helps keep airway clear if patient vomits.
Lying level ensures blood flow to brain.
Advise patient not to sit up or walk around, even during transport or feeling better.
Lay non-breathing patient on back for rescue breathing. Contact emergency medical care
TREATMENT FOR DCS
DCS treatment requires putting patient in a recompression chamber. Recompression reduces bubbles in body to a smaller size and forces them back into solution – often alleviates symptoms immediately. Treatment involves a long slow decompression with oxygen and drug therapy. Duration and need for drugs / oxygen makes attempting recompression in water very difficult, requiring manpower and special equipment.
The sooner recompression begins, the more likely the patient will recover without permanent injury. Patients sometimes don’t want to believe they are suffering from DCS and object to seeing a doctor. Strongly urge patients to allow medical examination by emergency medical care.
LUNG OVER-EXPANSION INJURIES
Lung over-expansion injuries are caused by:
Holding breath during ascent
Diving with a chest cold
Local blockage in the lungs due to loss of surfactant (due to smoking)
Expanding air over-expands and causes lung rupture
AIR EMBOLISM
Also called arterial gas embolism (AGE). Air enters the bloodstream and flows into arteries Serious and immediately life threatening. Bubbles can lodge anywhere, but the most common is to flow through the carotid arteries and cause cerebral air embolism, which can stop blood flow to parts of the brain depending on where in the arteries the embolus lodges)- there are some nice diagrams of the blood supply of the different territories of the brain which may be useful
Signs and symptoms (similar to a stroke)
- Dizziness
- Confusion
- Shock
- Paralysis (of face, arms or legs, usually one-sided)
- Personality change
- Unconsciousness and death
- Also Difficulty speaking or understanding other people
- Strange sensations like pins and needles or numbness
- Visual disturbance
PNEUMOTHORAX
Air from a rupture goes into the pleural space between the lung and chest wall causing the lung (or part of it) to collapse. Also serious.
Signs and symptoms
- Chest pain (particularly on breathing in), increasing breathlessness (these are the cardinal signs).
- Patient may cough up blood
MEDIASTINAL EMPHYSEMA
Air from the rupture accumulates in the centre of the chest, over the heart, causing pain in the middle of the chest, this is serious because air presses on the heart and vessels, interfering with circulation (affects ability of heart to pump effectively).
Signs and symptoms
- Patient may feel faint or short of breath.
SUBCUTANEOUS EMPHYSEMA
Air from a rupture accumulates in soft tissues under the skin usually at the base of the neck. The victim feels fullness in neck and voice may change.
Signs and symptoms
- The skin may crackle to the touch
FIRST AID
First Aid is the same as for DCS, hence the common term ‘decompression illness’ for both. Giving Oxygen helps supply tissues deprived of blood flow because of bubbles
Treatment of air embolism requires recompression to reduce bubble size (as with DCS). Importance of swift treatment in air embolism to reduce permanent damage to area of the brain which has been underperfused with oxygen
DCS OR DCI?
Decompression Sickness – nitrogen in the body coming out too fast
Decompression Illness – a collective term for decompression sickness and lung over-expansion injuries
SILENT BUBBLES
Some nitrogen dissolves into microscopic gas pockets in the body and form tiny bubbles that are trapped. These then diffuse harmlessly into air. Silent bubbles are found after some dives, especially those close to table / computer limits. These are larger bubbles than the tiny bubbles theorized to form after most dives, but are still harmless.
NITROGEN
Caused by breathing a high partial pressure of nitrogen. Using air or enriched air, narcosis is expected to be noticeable at about 30m depth. Helium is not narcotic even under very high pressures – this is why it is used by technical and commercial divers making very deep dives. Ascent (going to a shallower depth) relieves narcotic symptoms and usually has no after effects. Not directly hazardous – hazard comes from impaired judgement that may delay reactions or lead to poor decisions.
Breath Hold Diving and Apnea
During APNEA (breath-holding) the circulatory system uses oxygen stored in the lungs, muscles and blood to meet oxygen needs
BRADYCARDIA
In cool water, BRADYCARDIA (slowing of the heart) reduces circulation and is triggered by apnea (felt by cold on the face). Though this doesn’t appear to reduce oxygen consumption in humans (it does in marine mammals).
SHALLOW WATER BLACKOUT
You can increase breath-hold time by first hyperventilating (breathing deeply and rapidly) three or four times. This reduces circulatory carbon dioxide so it takes longer to get enough to cause breathing. Too much hyperventilation may lead to shallow water blackout. Occurs on ascent, near the surface. The reduced oxygen pressure prevents the haemoglobin bonding with oxygen so tissues and brain become starved of oxygen This is because the low carbon dioxide cannot stimulate breathing. It is the high carbon dioxide that stimulates the body to want to breath, not the lack of oxygen
CAROTID SINUS REFLEX
Carotid sinus receptors monitor pressure of arterial blood reaching the brain through the carotid arteries. Low blood pressure triggers a higher heart rate, and high blood pressure triggers a lower heart rate Receptors interpret pressure from an excessively tight hood or wet suit constricting the neck as high blood pressure. The heart rate slows, reducing blood flow to the brain, but pressure remains, causing yet slower heart rate. The diver feels uncomfortable and light-headed but may lose consciousness if constriction continues unrelieved.
Avoid by not wearing excessively tight hoods, wet suit or dry suit neck seals
HYPERCAPNIA
(Hyper = excess)
Hypercapnia is TOO MUCH carbon dioxide
Causes:
- Shallow rapid breathing
- Skip breathing (holding the breath periodically)
- Overexertion
- or a combination of these. In very rare cases air supply may be high in carbon dioxide.
- Respiratory drive impaired by head injury or drugs
- Trauma which causes respiratory muscle weakness
Signs and symptoms:
- Headache
- Accelerated breathing.
- Confusion
- Loss of consciousness
- early- flushed skin due to vasodilation, muscle- twitching, headache
- Progressing to disorientation, panic, convulsions, loss of consciousness..
Avoid by breathing deeply and normally, not skip breathing and by avoiding overexertion.
HYPOCAPNIA
(Hypo = too little)
Hypocapnia is NOT ENOUGH carbon dioxide
Too little carbon dioxide may interrupt the normal breathing cycle because carbon dioxide actually stimulates breathing.
Causes:
- Excessive hyperventilation (more than three or four breaths)
- This may be voluntary (quick breaths) or involuntary (due to stress or a fright while scuba diving) – causes light-headedness
Symptoms
- Light headedness
- Shallow water blackout>
- Visual disturbances
- Anxiety
- Pins and needles
- Muscle cramps especially in hands and feet
Visual disturbances, anxiety, pins and needles and muscle cramps especially in hands and feet
A diver ascends; the partial pressure drops and haemoglobin can no longer bond with oxygen. The diver blacks out without warning due to hypoxia (NOT ENOUGH OXYGEN)
CARBON MONOXIDE POISONING
Caused by contaminated and poor quality air. Smoking is another source of carbon monoxide. Carbon monoxide bonds more readily with haemoglobin than oxygen (by 200 times) but does not release as easily. Breathing air contaminated with carbon monoxide at depth, haemoglobin carries less and less oxygen as carbon monoxide bonds with it.
When a diver surfaces, plasma no longer can carry enough dissolved oxygen. The diver blacks out from hypoxia (NOT ENOUGH OXYGEN)
Signs and Symptoms of carbon monoxide include
- Headache
- Confusion
- Narrow vision
- Bright red lips / nails (not easily observed while underwater
Symptoms of mild cases subside after several hours of fresh air First Aid procedures: severe cases – give the diver 100% oxygen and contact emergency medical care.
OXYGEN TOXICITY (two types)
One involves the symptoms in the respiratory system, and the other involves the nervous system. Using enriched air nitrox (EANx) you can have oxygen toxicity.
CNS TOXICITY (most serious)
Central nervous system (CNS) oxygen toxicity involves nervous system reactions to oxygen exposure, and tends to be unpredictable, beyond the fact that it occurs at elevated oxygen partial pressures (greater than 1.4 bar / ATA)
Signs and Symptoms:
- Visual disturbances
- Ear ringing
- Nausea
- Twitching muscles
- Irritability
- Dizziness.
Further information
Most serious is convulsion (which cause a diver to drown)
Using normal air, a diver is risking CNS above 1.6 ATA at 66m.
On 100% oxygen a diver would reach a pp of 1.6 ATA at 6 meters.
CNS is considered life threatening in many diving situations because of sudden convulsions and unconsciousness.
Decongestants predispose you to CNS toxicity. Vitamin ‘E’, Valium and Magnesium are said to reduce the likelihood of CNS toxicity.
PULMONARY TOXICITY
Results from continuous exposure to an oxygen partial pressure greater than 0.5 bar / ATA.
Signs and Symptoms:
- Burning in the chest
- Irritated cough
Usually resolves itself by ceasing diving for several days. Not considered immediately life threatening or hazardous
HEAT EXHAUSTION
A condition in which the body works at full capacity to cool.
Signs and Symptoms:
- Weak, rapid breathing
- Weak rapid pulse
- Cool clammy skin
- Profuse sweating
- Dehydration
- Nausea
A diver with heat exhaustion should remove their exposure suit, seek shade, drink non-alcoholic fluids and rest until cool.
HEATSTROKE
A condition in which cooling has failed – an emergency medical condition (temp greater than 41 degrees)
Signs and Symptoms:
- Strong and rapid pulse
- No perspiration
- Skin flushed, hot to the touch
- Confusion
- Could lead to Brain damage, system damage or possible death
A diver with heatstroke should remove exposure suit and out the diver in a cool environment and contact emergency medical aid
HYPOTHERMIA
When core body temp drops below 35 degrees centigrade this Occurs when then diver ignores uncontrollable shivering or numbness and continues to cool Body temperature regulation mechanisms fail, the body core temperature drops and the shivering stops Diver may feel warm as blood rushes to skin – a dangerous condition because the diver doesn’t feel cold, but heat loss is now unchecked.
As the core temperature drops mental processes slow – diver becomes drowsy, uncoordinated and forgetful. Unchecked, hypothermia leads to unconsciousness, coma and death (when body temp reaches around 30 deg c). Advanced hypothermia is a medical emergency requiring emergency care.
Practice Exams – Theory and Standards
Dive Theory Exam D as well as PADI Dive Standards Exam D
Buy the complete IDC revision packs that now include lots more (another 10) practice exams, the exams include all the questions and answers you will need to revise to PASS the PADI IDC
